
When the United Nations meets Sept. 21 in New York, they want the UN to reframe its action on the global antimicrobial drug resistance (AMR) crisis.
It's crucial. How crucial is it?
Antimicrobial drug resistance threatens both personal and planetary health and the issue is as crucial as the global threat of climate change, Carroll says.
In a paper titled “Use Antimicrobials Wisely,” published in the current edition of Nature, a nine-member international research team, including Carroll, explained their advocacy.
“We're concerned about what will happen if the proposed UN solutions focus mainly on incentives for new drug development, at a time when the drug industry itself is abandoning those efforts against infectious disease due to AMR,” said Carroll, who co-leads the international group on resistance to pesticides and antimicrobial drugs. He founded and directs the Institute for Contemporary Evolution, Davis, and is affiliated with the Sharon Lawler lab, UC Davis Department of Entomology and Nematology.
The paper, published in the Comment section, is the first product from a two-year working group sponsored by the National Socio-Environmental Synthesis Center in Annapolis, Md. “We are taking a similar socio-environmental approach in our concurrent work on pesticide stewardship,” Carroll said.
“While new drugs have a role, we think it's more important for society to learn how to steward pathogen susceptibility, so we develop that theme in the paper,” Carroll said. “And because we also depend on microbes for digestion, immunity, and general health, and microbes support ecosystem functioning through nutrient cycles and the maintenance of soil and water quality, we further argue that our AM drug habits and waste streams threaten both personal and planetary health. “
Lead authors of the paper are Peter Jorgensen of Stockholm, Sweden, and Didier Wernli of Geneva Switzerland. Jørgensen, who spent part of his Danish graduate program working with Carroll in Davis, is now a postdoctoral researcher at the Royal Swedish Academy of Science, Stockholm.
Carroll described AMR as more than a medical dilemma—it's a socio-ecological problem. “The vulnerability of pathogens to antimicrobial drugs is a communal resource, readily threatened by overuse, to be lost as a classic 'tragedy of the commons.' There is a lot of contemporary theory for social resilience in the face of socio-ecological challenges, and– linking to entomology– the early success of the pioneering management of Bt crop pest resistance evolution is an encouraging precedent.”
In its planetary health approach, the group seeks to be “more cognizant not only of preserving drug susceptibility in pathogenic microbes, but also protecting from wholesale destruction the community of microbes on which we depend for life,” Carroll said.
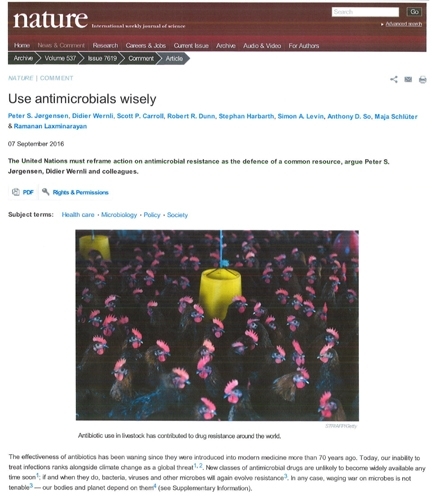
In the paper, the scientists pointed out that “Resistance affects animal and environmental health as well as human health, and so requires coordinated action across economic sectors. No single concern exemplifies this better than the high rate of antibiotic use in agriculture (largely as growth promoters or disease prevention).” They wrote that in the United States, 70 to 80 percent of all anti-microbials consumed are given to livestock.
An example of antimicrobial resistance involves the malaria mosquito, Anopheles gambiae. The World Health Organization (WHO) in a document, "Global Action Plan on Anti-Microbial Resistance," wrote:
"Antimicrobial resistance can affect all patients and families. Some of the commonest childhood diseases in developing countries – malaria, pneumonia, other respiratory infections, and dysentery – can no longer be cured with many older antibiotics or medicines. In lower- income countries, effective and accessible antibiotics are crucial for saving the lives of children who have those diseases, as well as other conditions such as bacterial blood infections. In all countries, some routine surgical operations and cancer chemotherapy will become less safe without effective antibiotics to protect against infections."
Expect to hear more about this alarming crisis--the global antimicrobial drug resistance crisis. Meanwhile, read the WHO Global Action Plan.
Attached Images:
